
This is a sign that respiratory effort is failing and that they are at risk of respiratory failure from fatigue. For patients on home oxygen, ask how many liters per minute they normally use, and if they have had to increase it recently.Ĭompromised exhalation from COPD may cause CO2 retention or hypercarbia. Both may be abnormal at baseline for COPD patients and many COPD patients know what their pulse-oximetry reading normally is. Measure pulse-oximetry and observe skin color to assess oxygenation. This helps determine initial treatment steps and anticipate the patient’s clinical course. Ask about what treatment they have used before you arrived, if their respiratory distress today is worse than it has ever has been before, and if they have ever been intubated for respiratory distress. Patients in severe respiratory distress may only be able speak in short phrases or nod their head yes or no to questions. Diminished or absent breath sounds indicates poor air movement through the lungs, and is an ominous sign.Īttempt to determine how the patient’s current respiratory status compares to their baseline. Patients with COPD may also exhale through pursed lips, which helps keep weakened alveoli open.Īuscultation of the lungs may reveal high pitched wheezes from air movement through constricted lower airways and low pitched, sonorous wheezes may be heard from air movement across mucus secretions. Supraclavicular and intercostal retractions indicate that the patient is using accessory muscles to breathe. 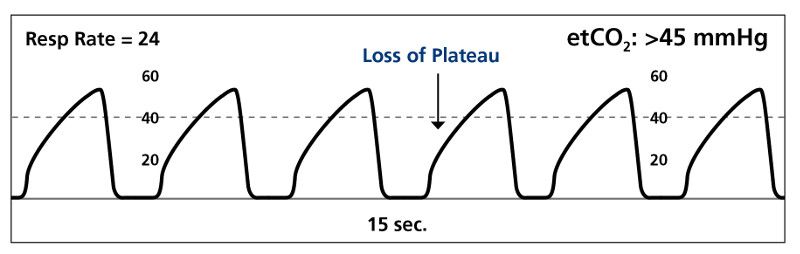
Patients in severe respiratory distress may be upright in a tripod position, and patients in respiratory failure may appear drowsy or unconscious. Observe the patient’s level of consciousness and position to assess their work of breathing. Understand how exam findings and point-of-care monitoring tools can be used. The onset of a COPD exacerbation may be sudden or gradual and patients may try to manage symptoms on their own for a long period before calling 911. COPD exacerbations may be triggered by noncompliance with a treatment plan, exposure to an allergen such as cigarette smoke or a respiratory infection. Patients with emphysema are often thin and have a barrel- shaped chest, pink and dry skin, and a dry cough.ĮMS is often called for exacerbations of COPD, which occurs when a patient’s baseline symptoms worsen. Once destroyed, several tiny alveolar sacs consolidate into one large sac, or bleb, which further decreases the surface area available for gas exchange. Trapped air causes the weakened alveoli to dilate, which eventually destroys the alveolar walls. This reduces the surface area available for oxygen diffusion on inhalation and prevents CO2-filled air from leaving the alveoli on exhalation. 
Patient with chronic bronchitis are often overweight, have cyanotic skin and have a frequent productive cough.Įmphysema causes the alveoli to lose elasticity. The bronchi are also hypersensitive to inflammation, which increases the frequency of sudden bronchoconstriction. In addition to the respiratory compromise caused by COPD, patients with COPD are at higher risk of pneumonia and right-sided heart failure.Ĭhronic bronchitis causes excess mucus to be secreted in the terminal bronchi, and impairs the cilia lining the terminal bronchi from clearing the secretions. The plan may include oral and inhaled medications to reduce bronchoconstriction and inflammation, as well as home oxygen to treat chronic hypoxia. 
Lung damage from COPD is irreversible, and people living with COPD have a prescribed treatment plan to manage their symptoms. Baseline respiratory status is compromised and declines further during COPD exacerbations. Here are five things EMS providers need to know about respiratory compromise from COPD: 1. ĬOPD exacerbations are frequently encountered by EMS providers, and proper assessment and treatment can significantly improve the patient’s respiratory status. Cigarette smoking is the most common cause of COPD, and chronic bronchitis and emphysema are the two main types. COPD includes a group of degenerative conditions that impair airflow through the lungs. Understand how monitoring tools can be used to guide treatment for COPD exacerbationsĬhronic obstructive pulmonary disease affects approximately 32 million Americans, and it is the fourth leading cause of death in the United States. January 27th, 2017 CapnoAcademy Articles, Learn Learn COPD exacerbation: 5 things EMS providers need to know
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
